News
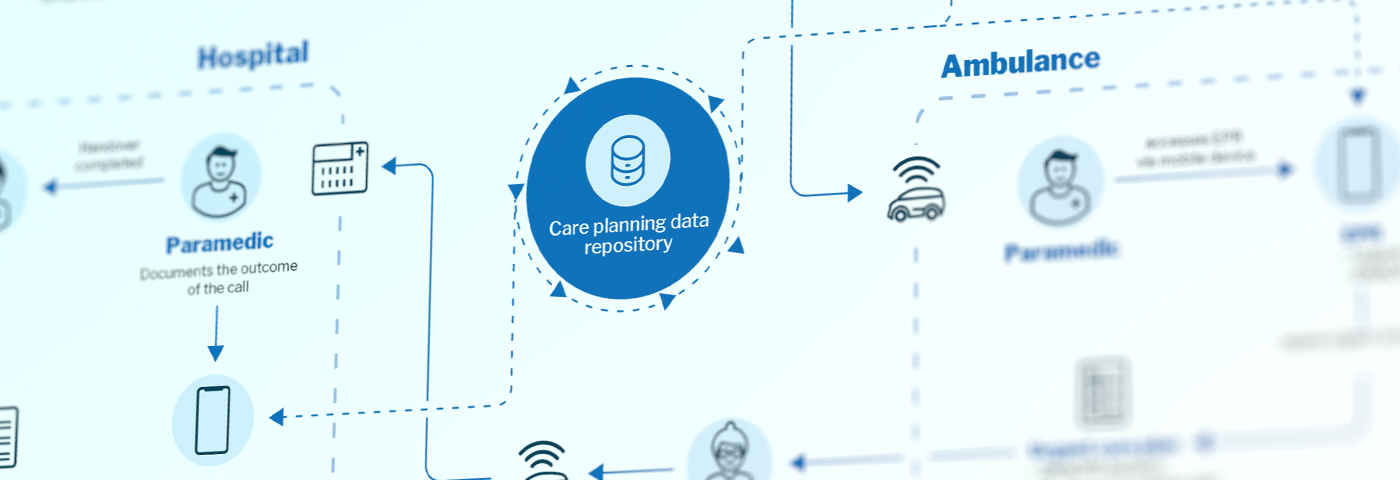
Digital health platforms give real time access to data and enable quick sharing of information
"Platforms standardise the way information is captured," said Gary McAllister, as a digital health platform with vendor-neutral data persistence, coupled with low-code tools, provides a huge opportunity for London to transform across the system. With the initial infrastructure connectivity in place that supports single organisations, alliances, and integrated care systems, it is likely to deliver digital services at scale and at pace.
As London embarks on a digital journey with Better, the software provider's Managing Director UK & Ireland Matt Cox was joined by OneLondon's CTO Gary McAllister at the Leading Health Innovation Summit to talk about the transformation of health and care across London using the Better platform.
OneLondon's vision is to provide digital health and care solutions in the region to enable London to become the healthiest city in the world. It will achieve this through sharing data, creating and promoting the use of digital standards and best practices, and with procuring and developing platforms that also support regional benefit.
Digital health platforms standardise the way information is captured
Why did OneLondon opt for the open platform approach? "They standardise the way information is captured and provide you with a controlled environment which gives tools, capability, and information modelling provision to information specialists and clinicians. They then bring together information into a standard set of tools to deliver to the point of care. There is also the other benefit to platforms, it gives real time access to information and enables other services to share the information more readily, and it has a standard attached to it – openEHR," explained Gary McAllister.
Matt Cox added that the main point here is the separation of data from applications and storing it in a vendor-neutral data repository, allowing London to be in control of its data, and then to extend this with data archetypes and modules as well as with the use of templates and forms. "We use openEHR standard, which is complementing FHIR and other standards across the system. And we use low-code to help organisations to accelerate the creation and delivery of applications and building e-forms, building data visualisations and dashboards," he added.
Data is the key to the conversation as there's often too much information at the point of care. As McAllister emphasised, the main point is to have access to data at the right place and the right time in the right data format. That is where the open data platforms come to the forefront. "We now have a partnership with Better initially focused on end-of-life care, which is about respecting an individual's needs at a time of the end of their life, and making sure that there is a direction of the conversation between the patient and the clinician. The patient feels in control and empowered through the process, as there is a continuous flow of communication between the clinician and the patient's wishes."
Having a single patient record has a real benefit
OneLondon's digital health strategy is beginning with the end-of-life care planning, but they want to expand it further. "Care planning by definition should be multi-agency," explained McAllister. "It shouldn't be just a single wait and see who has access to the care plan. They're an integral factor of all the elements of care. So, we have end-of-life. But we have a conversation about frailty, diabetes, other disciplines and diseases that require continuous care and improvement. And also, the pathways tend to span across ICSs in London, so having a single patient record that can actually be shared between agencies actually has a real benefit, especially when we talk about flows of documentation between the services".
"This approach works really well in the areas of complex data that's highly variable, such as end-of-life, participatory care and wider care planning with any number of different use cases making these structures and consistent data available through APIs to support other applications of national services, reducing data duplication and capture, which is frustrating for patients and citizens," said Matt Cox. "On top of this, we have low-code tools to create the care planning environment, able to design and launch new care plans. The difference we see in our approach is in the establishment of a platform to allow the rapid creation and continued development of digital services at scale across London," he added.
The project is now in the delivery phase. "We're doing all of the technical work required to integrate Better Platform at the point of care in pre-clinical design and clinical safety, working with a multitude of suppliers across our region, which provides the ability to have a context launch so you don't have to go searching for records. And it makes it easy to access. We hope to go live with it later this summer, early autumn, and beyond that, the London region will manage the government's records of information and capture services on top of the system itself," said McAllister.