healthcare
A glimpse into the future of seamless patient medication data exchange
For years, many clinicians have been dreaming about the day when making an accurate list of a patient’s medications on admission in the hospital would take a few minutes instead of hours, or days. In July, Better’s Better Meds team showed everyone how this very reality in our near future – where all medication-related systems in the UK will be connected – will look.

The complexity of creating complete medication reconciliation in hospitals comes from a lack of connectivity on several levels: between patient records kept by GPs and those stored in hospitals; between the medication lists of different hospitals (if a patient has been admitted to more than one); and between community pharmacies and hospitals.
Patients can also suffer because a poorly collected medication history can be the cause of medical errors. When visiting outpatient clinics, they might still need a paper prescription before picking up medications at a community pharmacy.
These are a recognised problems, and in the UK several efforts have been made to solve these issues through the use of connectivity standards: transfer of care for hospital-to-hospital data transfer, GP connect for connecting GP systems with other healthcare providers, and an Electronic Prescribing Service (EPS) to connect GP practices with community pharmacies.
The collaboration that drives faster innovation
On 14 and 15 July, INTEROPen – an action group aimed at accelerating the development of open standards for interoperability in the health and social care sector in the UK – organised a virtual hackathon for developers interested in designing a solution for medication interoperability across care settings. The winner was the team from Better which is building and developing Better Meds, a hospital electronic medication management system which has been chosen by five NHS Trusts in the UK, and two national speciality medical centres in Slovenia.
A glimpse of the future
At the hackathon, Better’s Better Meds team delivered a project which integrated Better’s prescribing and medication management system with a pharmacy integration standard, GP Connect, the Electronic Prescription Service, and transfer of care.
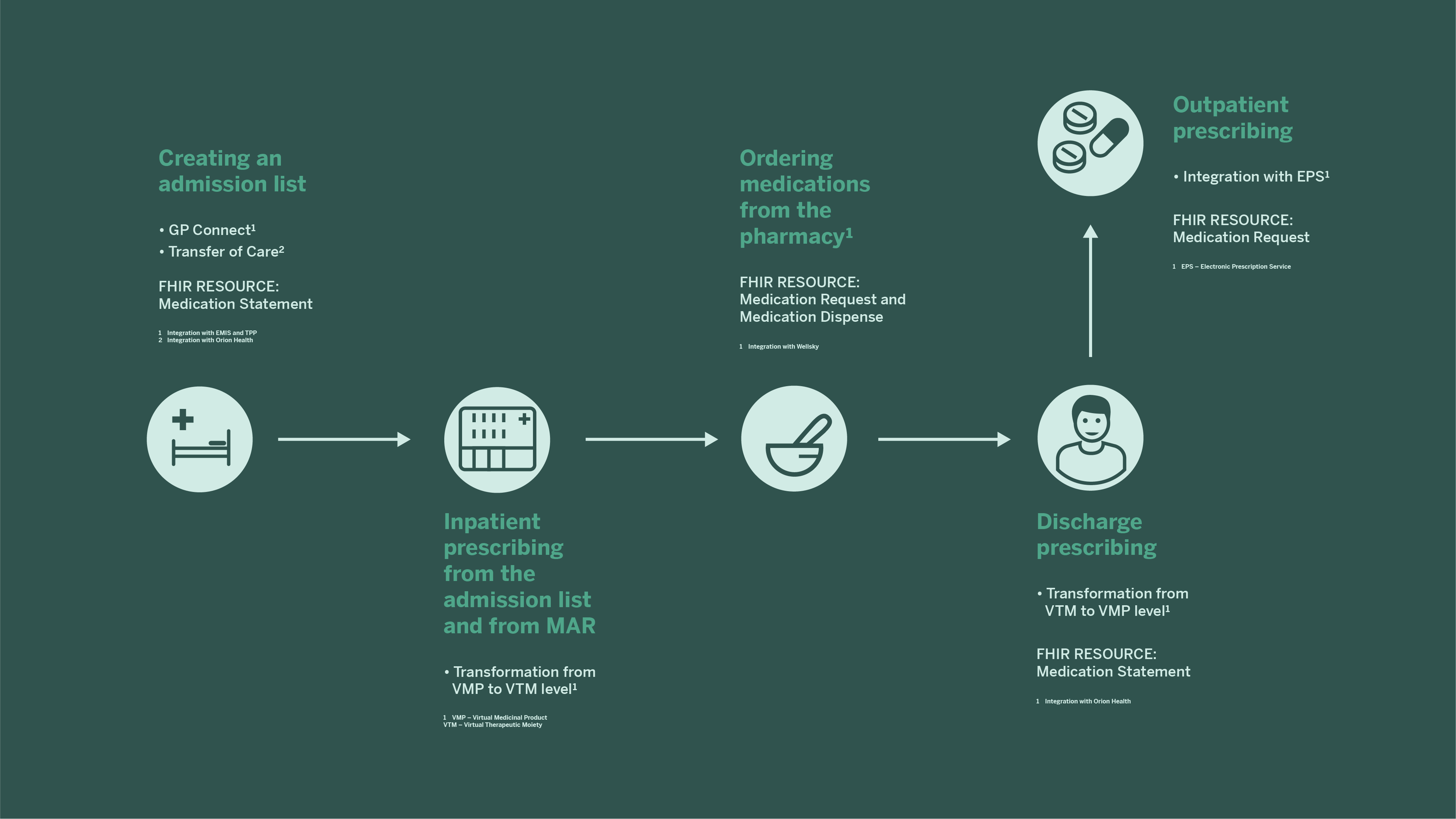
Healthcare development and medical progress are enhanced when time spent on tasks, such as gathering prescribing information, is reduced, and clinicians are then free to spend that time treating patients. With the use of the above-mentioned standards for medication information interoperability, healthcare in the UK is making one of many important steps towards its transformation into modern, connected healthcare, which will enable precise, personalised medicine.
The benefit for all of the teams involved at the hackathon, however, goes far beyond the benefits for UK healthcare. The team has proven the applicability of integration framework, and strategic importance of FHIR standard in achieving semantic interoperability on a global scale.
